Some people describe it as a bolt of lightning through the cheek. Others say it feels like being jabbed in the face with a hot poker — without warning, without mercy, and triggered by something as innocent as a morning breeze.
That’s tic douloureux: a nerve condition so severe it has earned a reputation as one of the most agonizing pain conditions a human being can experience. If you’ve recently felt unexplained electric shock facial pain or know someone who has, understanding this condition — what it is, what causes it, and how it’s treated — is the first step toward relief.
This guide covers everything you need to know, written from the perspective of a pain management practice that treats patients living with neuropathic facial pain every day.
What Is Tic Douloureux? (And What Does the Name Mean?)
The French Origin of “Tic Douloureux”
The name itself comes from French: tic meaning an involuntary muscle spasm or twitch, and douloureux meaning painful. The name captures exactly what clinicians first observed — patients wincing and flinching involuntarily as waves of intense pain crossed their face.
It’s an old term, dating back to the 18th century, but the condition it describes is as real and as debilitating as ever.
Tic Douloureux vs. Trigeminal Neuralgia — Is There a Difference?
Tic douloureux and trigeminal neuralgia are the same condition. The terms are used interchangeably in medical literature and clinical practice. “Trigeminal neuralgia” is the modern, anatomical name — referring to the trigeminal nerve, the fifth cranial nerve responsible for facial sensation. “Tic douloureux” is the older, French-derived term still widely used today, especially in patient conversations.
If you’ve been researching your symptoms and seen both terms, don’t let that confuse you. They describe the same disorder, the same pain, and the same treatment options.
To understand how this fits into the broader landscape of nerve-related pain, see our guide on types of chronic pain, including how neuropathic pain differs from other pain mechanisms.
What Does Tic Douloureux Feel Like? Trigeminal Neuralgia Symptoms
The Classic Lightning Bolt Pain Pattern
The hallmark of tic douloureux is sudden, severe, one-sided facial pain that most patients describe as an electric shock, a stab, or a lightning bolt. The pain is almost always unilateral — affecting only one side of the face — and it tends to strike in the jaw, cheek, lips, gums, or teeth.
Each episode typically lasts anywhere from a few seconds to two minutes. But attacks can cluster in rapid succession, sometimes dozens of times per day, creating what patients describe as an unbearable barrage.
Between episodes, there is usually no pain at all — which is one of the key clinical features that distinguishes tic douloureux from other chronic facial pain conditions.
Type 1 vs. Type 2 Trigeminal Neuralgia
Not everyone with this condition experiences the same pain pattern, which is why many people go undiagnosed for months or years.
Type 1 (TN1) is the classic presentation: sudden, sharp, shock-like attacks with complete pain-free intervals. This is the pattern most commonly described in medical literature.
Type 2 (TN2) involves a constant, lower-level aching or burning sensation that is present in the background, with occasional sharp attacks layered on top. This atypical form is less well-known but equally real — and equally disabling.
The Fear-Avoidance Cycle — When Pain Changes Your Behavior
One of the most underappreciated consequences of tic douloureux is what it does to daily life. Because pain can be triggered by the most ordinary activities, many patients begin to avoid them altogether.
They stop chewing on one side. They avoid smiling. They speak less. Some stop eating enough because meals become unbearable. This behavioral withdrawal can cause malnutrition, social isolation, anxiety, and depression — complications that compound the physical suffering significantly.
What Causes Tic Douloureux? Understanding Facial Nerve Pain
Blood Vessel Compression (Most Common Cause)
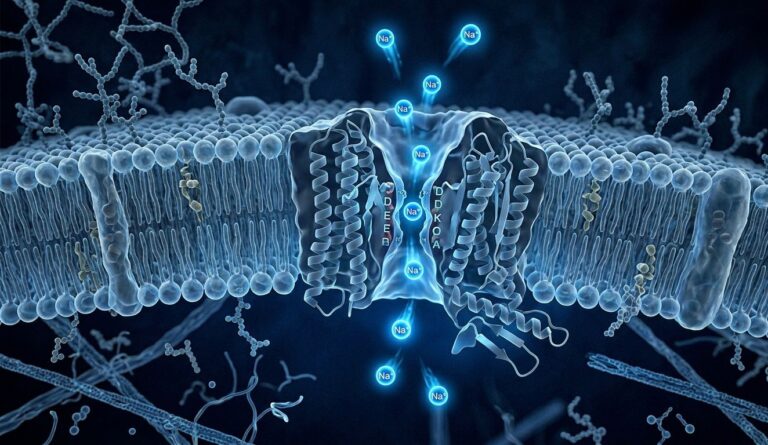
The most widely accepted explanation for tic douloureux involves vascular compression — an abnormal blood vessel pressing against the trigeminal nerve near its root. Over time, this pressure erodes the myelin sheath, the protective coating around the nerve. A damaged myelin sheath causes the nerve to misfire, sending spontaneous pain signals that the brain interprets as extreme facial pain.
This is why, in many cases, surgery can provide lasting relief: removing the compressing vessel from the nerve stops the erratic firing at its source.
Multiple Sclerosis and Other Neurological Causes
In a smaller subset of patients, tic douloureux is secondary to another neurological condition. Multiple sclerosis (MS), for example, can demyelinate portions of the trigeminal nerve, producing identical symptoms. Other causes include tumors pressing on the nerve, arteriovenous malformations, or trauma to the face or skull.
Because of the MS connection, trigeminal neuralgia in a younger patient — particularly one under 40 — should prompt evaluation for underlying demyelinating disease.
Who Is Most at Risk?
Tic douloureux most commonly appears in people over 50, and it affects women slightly more often than men. Approximately 15,000 new cases are diagnosed in the United States each year. People with multiple sclerosis have a significantly elevated risk compared to the general population.
Common Triggers of Electric Shock Facial Pain
One of the most distressing aspects of this condition is that the triggers are completely ordinary. Pain attacks can be set off by:
- Chewing or eating (especially hard foods)
- Talking or laughing
- Cold air hitting the face
- Brushing or touching the teeth
- Touching the face gently
- Shaving or applying makeup
- Smiling
Why Even Light Touch Can Cause Agony
These triggers operate through what are called “trigger zones” — small areas on the face, lips, gums, or nose that, when stimulated, fire a pain episode. What makes this neurologically remarkable is that light touch — the kind that shouldn’t hurt at all — causes more severe pain than firm pressure in many patients.
This phenomenon, known as allodynia, is a signature of nerve-driven pain and helps clinicians distinguish tic douloureux from dental pain, sinus pressure, or other facial conditions with overlapping symptoms.
How Is Tic Douloureux Diagnosed?
There is no single blood test or imaging study that definitively confirms tic douloureux. Diagnosis is primarily clinical — based on a detailed description of the pain, its pattern, its triggers, and its location.
Neurological Examination
A neurologist or pain specialist will evaluate your reflexes, facial sensation, and the distribution of your pain. The characteristic features — unilateral location, episodic shock-like quality, trigger zones — form a clinical picture that is often distinctive enough to make a working diagnosis.
MRI and Imaging
An MRI of the brain and brainstem is typically ordered to look for vascular compression of the trigeminal nerve root, rule out MS plaques, and identify any tumors or structural abnormalities that might be causing secondary trigeminal neuralgia. High-resolution MRI with special sequences can sometimes directly visualize a blood vessel in contact with the nerve.
Ruling Out Other Conditions
Because tic douloureux pain often affects the jaw, cheek, and teeth, many patients first see a dentist — and sometimes undergo unnecessary dental procedures before the neurological origin of the pain is recognized. Cluster headaches, dental abscess, temporomandibular joint (TMJ) disorder, and atypical facial pain can all mimic aspects of the condition.
A thorough evaluation by a pain specialist helps rule these out and confirm the diagnosis.
Tic Douloureux Treatment: From Medication to Surgery
First-Line Medications — Carbamazepine and Beyond
The cornerstone of tic douloureux treatment is pharmacological. Carbamazepine (Tegretol) is the most well-established first-line medication and is specifically FDA-approved for trigeminal neuralgia. It works by stabilizing overactive nerve membranes, reducing the frequency and intensity of pain episodes.
Many patients experience significant relief initially. However, carbamazepine carries potential side effects — drowsiness, dizziness, and in some cases liver or bone marrow issues — that require monitoring with bloodwork.
When carbamazepine is not tolerated, alternatives include oxcarbazepine (which has a similar mechanism with a somewhat better side-effect profile), gabapentin, baclofen (especially when used in combination), and lamotrigine. For detailed, authoritative information on medication options, the Mayo Clinic’s trigeminal neuralgia treatment overview is an excellent reference.
When Medications Stop Working
Over time, many patients find that medications become less effective or cause side effects severe enough to limit their use. This is a known pattern — the condition tends to progress, with episodes becoming more frequent and more resistant to pharmacological management.
This is the point at which a referral to a pain specialist or neurosurgeon becomes important. There are effective interventional and surgical options that many patients don’t know are available.
Surgical Options — Microvascular Decompression (MVD)
Microvascular decompression is considered the most durable surgical treatment for tic douloureux caused by vascular compression. During the procedure, a neurosurgeon accesses the posterior fossa through a small opening behind the ear and places a tiny cushion — usually a Teflon pad — between the offending blood vessel and the trigeminal nerve.
Because it addresses the root cause rather than destroying or damaging the nerve itself, MVD carries the highest long-term success rates of any surgical option, with many patients experiencing complete, lasting relief. It does require general anesthesia and a brief hospital stay, which makes patient selection and preoperative evaluation essential.
Stereotactic Radiosurgery (Gamma Knife)
For patients who are not surgical candidates due to age, medical comorbidities, or personal preference, stereotactic radiosurgery — commonly called Gamma Knife radiosurgery — offers a non-invasive alternative. This technique delivers a highly focused beam of radiation to the trigeminal nerve root, gradually reducing its ability to transmit pain signals.
Results typically develop over weeks to months. It is less immediately effective than MVD but carries minimal procedural risk, making it particularly appropriate for older or medically fragile patients.
Other percutaneous procedures — including glycerol rhizotomy and balloon compression — are also available and may be appropriate depending on the individual patient’s clinical situation.
When Should You See a Pain Specialist for Tic Douloureux?
Many patients with tic douloureux spend months seeing dentists, ENTs, or primary care physicians before receiving an accurate diagnosis. If you are experiencing any of the following, it is time to seek evaluation from a pain specialist or neurologist:
- Recurrent episodes of one-sided, electric shock-like facial pain
- Pain that is triggered by eating, talking, or light touch
- Facial pain that has not responded to dental treatment
- Worsening pain despite medication
- Facial pain alongside other neurological symptoms (numbness, weakness, vision changes)
At Advanced Spine and Pain, our specialists evaluate and treat complex neuropathic pain conditions across our locations in Virginia, Maryland, and Delaware. Our approach combines accurate diagnosis with a personalized treatment plan — from medication management to referral for surgical options when appropriate. You can also review our pain management services to understand the full scope of care we offer. If you’re curious about how chronic pain is classified and why the type of pain matters so much for treatment, our article on types of chronic pain is a helpful starting point.
Frequently Asked Questions About Tic Douloureux
Is tic douloureux the same as trigeminal neuralgia?
Yes. They are two names for the exact same condition. Trigeminal neuralgia is the modern clinical term. Tic douloureux is the older French name historically used to describe the involuntary facial twitching that accompanies severe pain attacks.
What causes electric shock facial pain?
The most common cause is a blood vessel pressing on the trigeminal nerve near the brainstem, which disrupts the nerve’s protective myelin sheath and causes it to fire erratically. Less commonly, the cause includes MS, tumors, or facial trauma.
Can tic douloureux be cured?
It cannot always be permanently eliminated, but it can be very effectively managed. Many patients achieve long-term or complete pain relief with surgery, particularly microvascular decompression. Medications control symptoms for many others. Working with a specialist to find the right treatment approach is essential.
Is tic douloureux dangerous?
It is not life-threatening in most cases. However, the severity of the pain and the behavioral changes it causes — including fear of eating, social withdrawal, and depression — can have serious consequences for overall health and quality of life. The condition warrants prompt evaluation and active management.
Conclusion
Tic douloureux is not “just” facial pain. It is one of the most severe pain syndromes in all of medicine — one that can reshape a person’s daily life around the fear of the next attack. But it is also one of the most treatable neuropathic pain conditions, with an established pathway from diagnosis through medication to surgery that produces meaningful relief for the vast majority of patients.
If you or someone you care about is experiencing recurrent, shock-like facial pain, don’t wait. The specialists at Advanced Spine and Pain are here to help you find answers — and a path forward. Request an appointment today.